

This therapist directory is offered in partnership with BetterHelp. If you sign up for therapy after clicking through from this site, HelpGuide will earn a commission. This helps us continue our nonprofit mission and continue to be there as a free mental health resource for everyone.
Need to talk to someone now? Find a crisis helpline
If you're a BetterHelp therapist with questions about your directory listing, please contact therapists@betterhelp.com
Loud snoring—especially accompanied by daytime sleepiness—may be a sign of obstructive sleep apnea, a serious sleep disorder. Here’s how to recognize the signs and get the right sleep apnea treatment.

Sleep apnea is a sleep disorder in which your breathing is repeatedly interrupted during sleep. These breathing pauses typically last between 10 to 20 seconds and can happen from 5 to over 100 times per hour.
The lack of oxygen during a sleep apnea episode jolts you awake—usually so briefly that you don’t remember it. But these disruptions to your natural sleep rhythm mean that you spend more time in light sleep and less in the deep, restorative sleep you need to be energetic, mentally sharp, and productive the next day.
Sleep apnea can also cause many health problems—in some cases deadly. So it’s important to take seriously. If you or your bed partner suspect sleep apnea, talk to your doctor without delay.
Obstructive sleep apnea (OSA) is the most common type of sleep apnea (and is the primary focus of this article). It occurs when the muscles that support the soft tissues in the upper airway relax during sleep and block the normal flow of air in and out of the nose and mouth. This usually causes loud snoring and interrupted breathing.
Central sleep apnea is a much less common type of sleep apnea that involves the central nervous system. It occurs when the brain temporarily stops sending signals to the muscles that control breathing. It is often caused by an underlying health condition. People with central sleep apnea seldom snore.
Complex or mixed sleep apnea is a rare combination of obstructive sleep apnea and central sleep apnea.
As airflow stops during a sleep apnea episode, the oxygen level in your blood drops. Your brain responds by briefly disturbing your sleep enough to kick start breathing—which often resumes with a gasp or a choking sound. If you have obstructive sleep apnea, you probably won’t remember these awakenings. Most of the time, you’ll stir just enough to tighten your throat muscles and open your windpipe. In central sleep apnea, you may be conscious of your awakenings.
BetterHelp is an online therapy service that matches you to licensed, accredited therapists who can help with depression, anxiety, relationships, and more. Take the assessment and get matched with a therapist in as little as 48 hours.
Take Assessment HelpGuide is user supported. We earn a commission if you sign up for BetterHelp’s services after clicking through from this site. Learn moreIt can be tough to identify sleep apnea on your own, since the most prominent symptoms only occur when you’re asleep.
But you can get around this difficulty by asking a bed partner to observe your sleep habits, or by recording yourself during sleep. If pauses occur while you snore, and if choking or gasping follows the pauses, these are major sleep apnea warning signs.
Not everyone who snores has sleep apnea, and not everyone who has sleep apnea snores. So how do you tell the difference between normal snoring and a more serious case of sleep apnea?
The biggest telltale sign is how you feel during the day. Normal snoring doesn’t interfere with the quality of your sleep as much as sleep apnea does, so you’re less likely to suffer from extreme fatigue and sleepiness during the day. The way you sound when you’re snoring also provides clues. As mentioned above, if you’re gasping, choking, or making other unusual sounds, you should suspect sleep apnea.
Keep in mind that even if you don’t have sleep apnea, a snoring problem can get in the way of your bed partner’s rest and affect your own sleep quality. But there are tips and treatments that can help you stop snoring.
While anyone can have sleep apnea, certain factors increase the risk:
Allergies or other medical conditions that cause nasal congestion and blockage can also contribute to sleep apnea.
Like obstructive sleep apnea, central sleep apnea is more common in men and people over the age of 65. But unlike obstructive sleep apnea, central sleep apnea is often associated with serious illness, such as heart disease, stroke, neurological disease, or spinal or brainstem injury. Some people with obstructive sleep apnea can also develop central sleep apnea when they’re being treated with positive airway pressure (PAP) devices.
The chronic sleep deprivation caused by sleep apnea can result in daytime sleepiness, fatigue, difficulty concentrating, forgetfulness, and an increased risk of accidents and errors in your daily activities.
Sleep apnea also has a mental impact. It can trigger moodiness and irritability and cause anxiety and depression. It also increases your risk of other serious health problems like high blood pressure, heart disease, diabetes, atrial fibrillation, and stroke.
In order to find out of if you have sleep apnea, you’ll need to see a doctor—preferably a sleep medicine specialist. They will evaluate your symptoms, take your medical history, and perform a sleep study.
A sleep study known as a polysomnogram is still the gold standard for diagnosing sleep apnea. It’s conducted in a hospital or sleep lab, where you’ll be hooked up to sensors and monitored overnight (or sometimes for two partial nights). However, many people are now able to be tested in the comfort of their own home using portable monitors that measure heart rate, breathing, and oxygen in the blood while you sleep.
A sleep apnea diagnosis is made based on the number of breathing episodes you experience per hour of sleep, as shown by your sleep study, as well as symptoms such as snoring and daytime sleepiness.
According to the American Academy of Sleep Medicine, sleep apnea is classified from mild to severe based on how many times you stop breathing:
It can be scary to receive a sleep apnea diagnosis. But the good news is that it’s treatable. And for most, treatment makes an enormous difference in the way they feel, both mentally and physically.
For mild cases of sleep apnea, lifestyle changes may be enough to treat the issue. Your doctor will let you know if that’s the right starting point. But even if you are prescribed a medical treatment, the following changes can help reduce your sleep apnea episodes and improve your sleep.
Lose weight. If you are overweight, losing weight can have an enormous impact. While it is usually not a total cure, it can reduce the number of breathing episodes you experience, reduce your blood pressure, and decrease daytime sleepiness. Even a small amount of weight loss can open up your throat and improve sleep apnea symptoms.
[Read: How to Lose Weight and Keep it Off]
Exercise. Even when exercise does not lead to weight loss, it can decrease your sleep apnea breathing episodes and improve your alertness and energy during the day. Aerobic exercise, resistance training, and yoga are all good choices for strengthening the muscles in your airways and improving breathing.
[Read: How to Start Exercising and Stick to It]
Sleep on your side. Lying on your back is the worst position for sleep apnea, as it causes the jaw, tongue, and other soft tissues to drop back toward the throat, narrowing your airway. Sleeping on your stomach isn’t much better, since lying face down or twisting your head to the side both obstruct breathing. Lying on your side, on the other hand, helps keep your airway open. If you find side sleeping uncomfortable or you tend to roll on to your back after you’re asleep, contoured side pillows or body pillows may help. You can also find mattresses that are ideal for side sleepers.
Avoid alcohol, anti-anxiety medication, and other sedatives, especially before bedtime, because they relax the muscles in the throat and interfere with breathing. This includes benzodiazepines (e.g. Xanax, Valium, Klonopin, Ativan), antihistamines (e.g. Benadryl, Claritin), opiates (e.g. morphine, codeine, Vicodin, Percocet), and sleeping pills.
Prop your head up. Elevate the head of your bed by four to six inches, or elevate your body from the waist up by using a foam wedge or special cervical pillow. Using the incline feature of an adjustable bed can also help.
Open your nasal passages at night by using a nasal dilator, saline spray, breathing strips, or a nasal irrigation system (neti pot).
Quit smoking. Smoking contributes to sleep apnea by increasing inflammation and fluid retention in your throat and upper airway.
Avoid caffeine and heavy meals within two hours of going to bed.
In addition to lifestyle changes, most people with sleep apnea will need to seek treatment that helps keep the airway open during sleep. Currently, the most effective treatment for mild to severe sleep apnea is continuous positive airflow pressure — or CPAP — therapy.
A CPAP device is a machine that uses a hose and airtight nosepiece or mask to deliver a steady stream of air as you sleep. The air pressure helps keep your airway open, preventing pauses in breathing.
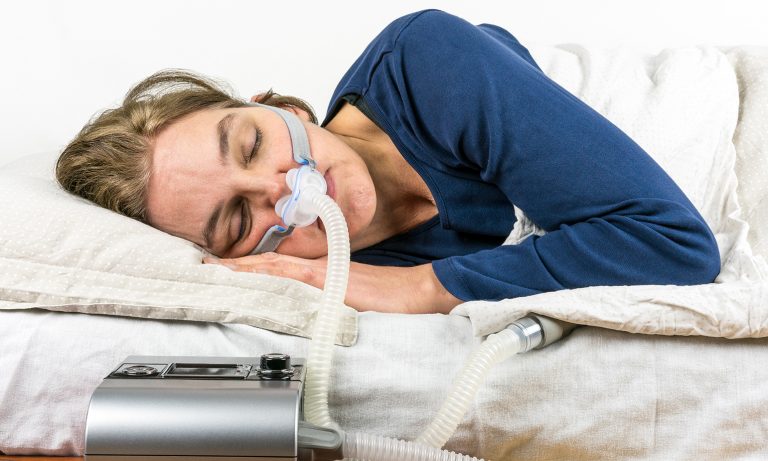
Some people have trouble sleeping with a CPAP device. But after an adjustment period, most people learn to sleep comfortably. In many cases, you’ll experience immediate symptom relief and a huge boost in your mental and physical energy, so it’s worth giving CPAP therapy a true shot.
CPAP technology is constantly being updated and improved, and the new CPAP devices are lighter, quieter, and more comfortable than they used to be. So even if you’ve given up on them in the past, you owe it to yourself to give them a second look.
It can take some time to get accustomed to sleeping while wearing a CPAP device. It’s natural to miss sleeping the “old way,” but there are things you can do to make the adjustment easier and to ensure you’re getting the most benefit out of treatment.
When it comes to CPAP therapy, one size does not fit all. It’s very important to get a mask that fits correctly and is comfortable for you.
There are many different types of masks available, including ones that cover the full face and ones that cover only the nose. Masks also come in a range of sizes, to accommodate different face shapes. There are also options that allow you to sleep in any position, accommodate glasses, and stay on if you toss and turn.
Be sure to discuss your options with your doctor and schedule follow-up appointments to check the fit, evaluate your treatment progress, and adjust or switch your mask if necessary.
Ease into it. Start by using your CPAP device for short periods. Try wearing it for a half hour or an hour while sitting up in bed watching TV or reading a book. Once you’ve gotten used to that, try using it lying down or when napping.
Use the “ramp” setting. Most devices can be programmed to start slowly and gradually increase air pressure. The goal is to be asleep before the machine reaches your prescribed pressure setting. Most people find this makes falling asleep much easier and more comfortable.
Reset the machine if air flow wakes you. If a high-pressure stream of air wakes you up, turn the CPAP device on and off to restart the ramp setting.
Choose a CPAP device with a built-in humidifier. Most devices now include a built-in humidifier, which helps prevent the dryness and skin irritation that can sometimes occur.
If you’re experiencing nasal congestion, you may prefer a full-face mask over a nasal or nasal pillow mask. Also be sure to keep your humidifier tank full, keep your tubing and mask clean, and make sure your filter is clean. Nasal sprays and antihistamines also help.
Keep your device clean. It’s very important to clean your CPAP hose, nosepiece or mask, and humidifier tub regularly, as a dirty CPAP device can cause infections and even pneumonia. Your sleep doctor and device manufacturer will give you detailed cleaning instructions.
To ensure maximum comfort, ask your doctor about soft pads to reduce skin irritation, nasal pillows for nose discomfort, and chinstraps to keep your mouth closed and reduce throat irritation and dry mouth.
Mask the sound of the CPAP machine. Most new CPAP devices are quiet, but if the sound of your CPAP machine bothers you, try placing it beneath the bed and using a sound machine to muffle the noise.
In addition to CPAP, there are other devices that a sleep specialist may recommend for sleep apnea treatment.
Expiratory positive airway pressure (EPAP) single-use devices fit over the nostrils to help keep the airway open and are smaller, less intrusive than CPAP machines. These may benefit people with mild-to-moderate obstructive sleep apnea.
Bilevel positive airway pressure (BiPAP or BPAP) devices can be used for those who are unable to adapt to using CPAP, or for central sleep apnea sufferers who need assistance for a weak breathing pattern. This device automatically adjusts the pressure while you’re sleeping, providing more pressure when you inhale, less when you exhale. Some BiPAP devices also automatically deliver a breath if the mask detects that you haven’t taken one for a certain number of seconds.
Adaptive servo-ventilation (ASV) devices can be used for treating central sleep apnea as well as obstructive sleep apnea. The ASV device stores information about your normal breathing pattern and automatically uses airflow pressure to prevent pauses in your breathing while you’re asleep.
Custom-made oral appliances are an increasingly popular means of treatment for sleep apnea. While not as effective as CPAP therapy, they are a good option if you can’t tolerate wearing a CPAP device, as most people find them more comfortable.
While there are many different oral appliances approved for sleep apnea treatment, most are either acrylic devices that fit inside your mouth, much like an athletic mouth guard, or fit around your head and chin to adjust the position of your lower jaw.
Two common oral devices are the mandibular advancement device and the tongue retaining device. These devices open your airway by bringing your lower jaw or your tongue forward during sleep.
Since there are so many different devices available, it may take some experimentation to find the appliance that works best for you. It’s also very important to get fitted by a dentist specializing in sleep apnea, and to see the dentist on a regular basis to monitor any problems and periodically adjust the mouthpiece.
There are some potential side effects to oral appliances, including soreness, saliva build-up, and damage or permanent change in position of the jaw, teeth, and mouth. These could be more serious in poorly fitted devices.
One of the newest treatments for sleep apnea involves the insertion of a pacemaker system that stimulates muscles to keep airways open so you can breathe during sleep.
The system involves three small components—a generator, a breathing sensor lead, and a stimulation lead—all of which are implanted in the neck and chest during outpatient surgery. You activate it each night with a remote and turn it off when you wake.
The new treatment has been approved by the FDA in the U.S. for people with moderate to severe obstructive sleep apnea. Research shows it improves the quality of life in these patients as their sleep issues decrease. It’s not approved for use in cases of central sleep apnea.
Major insurance providers and Medicare may cover the treatment; however, certain conditions may need to be met. For example, you must have previously tried CPAP to manage moderate or severe OSA. Your body max index (BMI) may also be a factor in determining whether your insurance will pay for the treatment. If your BMI is below 32, an insurance company is more likely to pay for the therapy than if your BMI is higher. Check in with your provider to determine if the cost of the treatment will be reimbursed.
If you have exhausted other sleep apnea treatment options, surgery to increase the size of your airway may be a possibility.
The surgeon may remove tonsils, adenoids, or excess tissue at the back of the throat or inside the nose, reconstruct the jaw to enlarge the upper airway, or implant plastic rods into the soft palate. Surgery carries risks of complications and infections, and in some rare cases, symptoms can become worse after surgery.
While obstructive sleep apnea can be common in children, it’s not always easy to recognize. In addition to continuous loud snoring, children with sleep apnea may:
If you suspect sleep apnea in your child, it’s important to consult a pediatrician who specializes in sleep disorders. Left untreated, sleep apnea can affect your child’s learning, mood, growth, and overall health.
The most common causes of obstructive sleep apnea in kids are enlarged tonsils and adenoids. A simple adenotonsillectomy to remove the tonsils and adenoids usually corrects the problem. Your child’s doctor may also recommend using a CPAP or other breathing device.
If excess weight is causing your child’s obstructive sleep apnea, your support, encouragement, and positive role modeling can help your child reach and maintain a healthy weight — and get your whole family on a healthier track.
Millions of readers rely on HelpGuide.org for free, evidence-based resources to understand and navigate mental health challenges. Please donate today to help us save, support, and change lives.
Donate to HelpGuide.org today